CendR Platform® – Targeted penetration technology to enhance drug delivery to advanced solid tumors
Advanced solid tumor cancers are types of cancer that have spread beyond the primary cancer site. The tumors in these advanced cancers can also recur after treatment. These solid cancers are often more difficult to treat in patients than cancer with an earlier stage tumor because they have progressed further.
Breast, colorectal, pancreatic, and lung cancer are common types of advanced solid tumor cancers. Typical treatment options for patients with advanced solid tumors may include surgery, chemotherapy, radiation therapy, targeted therapy, and immunotherapy. Lisata’s CendR Platform® is designed to enable more effective tumor-targeted, tissue penetrating delivery of anti-cancer drugs to solid tumors.
The CendR Platform® has the potential to revolutionize the way we treat advanced solid tumors, and could ultimately lead to more successful outcomes for patients.
What is the tumor microenvironment (“TME”)?
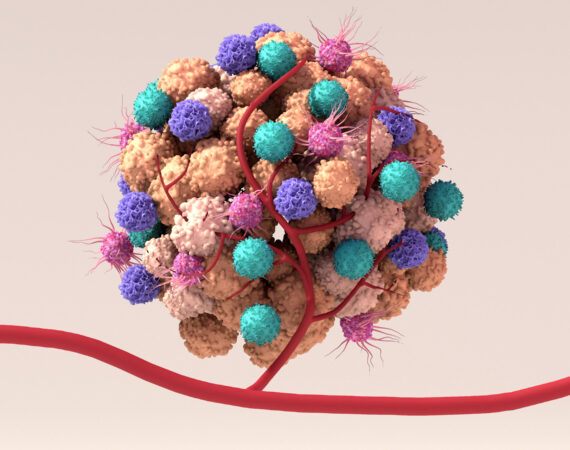
In the world of anti-cancer research, directly targeting tumor cells is one challenge; penetrating the cells to deliver therapeutics is another. Solid tumors are complex organ-like structures; The tumor microenvironment (“TME”) describes the entirety of the tumor components that are not malignant by themselves. The TME consists of the tumor’s vasculature, connective tissue (stromal cells), infiltrating immune cells, and the extracellular matrix (or “ECM”). The ECM is a non-cellular meshwork of crosslinked macromolecules that form a dense desmoplastic stroma around tumor cells. This complex meshwork, together with the formation of new collapsed and leaky blood vessels, creates a TME in favor of tumor growth and invasiveness. Thus, the presence of ECM, poor and tortuous vascularity of the tumor, as well as high interstitial tumor pressure may cause, in some cases, only a small fraction of an administered anti-cancer drug to cross this dense desmoplastic stroma barrier and reach the tumor. The TME can also prevent extravasation of immune cells into the tumor. Additionally, the TME in many tumors can be populated with immune and other non-cancerous cells that establish an immunosuppressive environment that can protect the tumor from attack by a patient’s immune system or by immunotherapies. Cell types, including cancer-associated fibroblasts (“CAFs”), T regulatory cells (“Tregs”), and tumor-associated macrophages (“TAMs”) can send signals by secreting classes of immunosuppressive cytokines that inhibit immune response to the presence of cancerous cells. The combination of specific targeting and efficient delivery could lead to highly effective cancer therapy in patients.
The CendR Platform®: Advancing Solid Tumor Treatment
The CendR Platform® incorporates novel technologies to enable more effective tumor-targeted, tissue penetrating delivery of anti-cancer drugs to solid tumors. The Platform can also target non-cancerous, immunosuppressive cells selectively within the tumor to enable a patient’s immune system and/or immunotherapies to fight cancer more effectively.
Lisata’s lead product candidate: Certepetide for the treatment of Pancreatic Cancer and Other Advanced Solid Tumors
Lisata’s proprietary CendR Platform® technology has led to the development of its lead investigational drug, certepetide, for the treatment of pancreatic cancer and other difficult-to-treat advanced solid tumors.
Certepetide is an investigational drug that is intended to modify the tumor microenvironment. It targets tumor vasculature by its affinity for alpha-v integrins that are selectively expressed in tumors, but not in healthy tissue vasculature. Certepetide is a cyclic peptide that, once bound to these integrins, is cleaved by proteases expressed in tumors.
Once cleaved to a linear peptide fragment, called a CendR fragment, CendR binds to a second receptor, called neuropilin-1, to activate a novel uptake pathway that allows anti-cancer drugs to penetrate solid tumors more efficiently and selectively.
The ability of certepetide to modify the TME to enhance delivery and efficacy of co-administered drugs has been demonstrated in models of a range of solid tumors. Certepetide has also been shown to decrease the percentage of immunosuppressive Tregs and to increase the percentage of cancer fighting CD8+ T cells selectively within the tumor in animal models of pancreatic cancer.
The Lancet Gastroenterology and Hepatology published encouraging data from the Phase 1 study of certepetide in combination with gemcitabine and nab-paclitaxel for the treatment of first-line, metastatic pancreatic ductal adenocarcinoma (mPDAC).
The publication details the results of an open-label, multi-center, Phase 1 trial conducted in 31 patients in the safety population and 29 patients in the efficacy population.
The objectives of the study were to determine the safety, tolerability, pharmacokinetics, and preliminary efficacy of certepetide in combination with gemcitabine and nab-paclitaxel in patients with mPDAC. Lisata and collaborators are exploring additional applications of certepetide to treat additional solid tumor types and combinations, including immunotherapies.